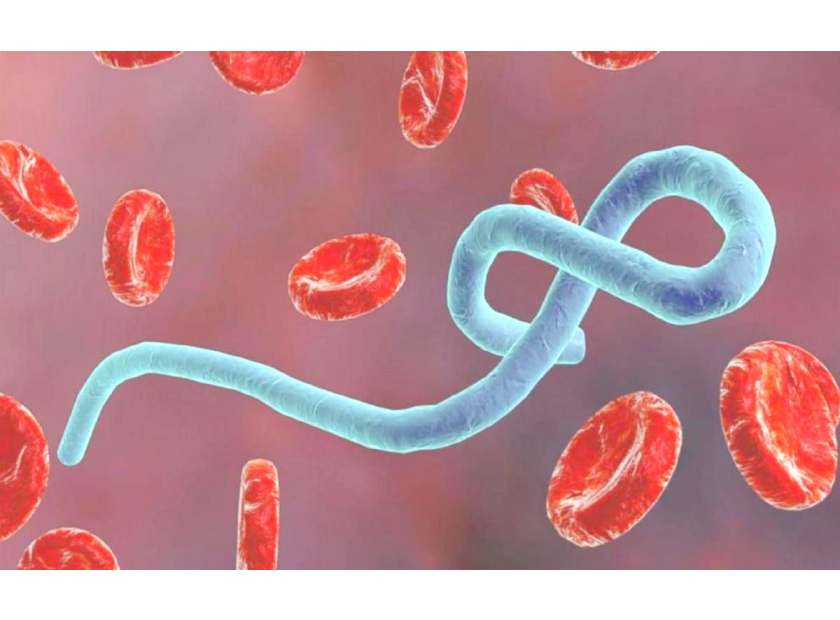
Is there a simple and inexpensive treatment for Ebola?
Antidepressants may be our best bet in treating Ebola
The 2013 to 2016 Ebola outbreak in West Africa made global headlines and inflamed discussion as the largest single outbreak of this deadly virus. The lack of a vaccine approved for use in humans and the rapid rate of mutation in the Ebolavirus genus create a particular vulnerability to large-scale outbreaks. While vaccination development focuses on traditional antiviral approaches, screens of FDA-approved drugs have shown that a multitude of agents will inhibit the progression of Ebola to varying degrees. A University of Oxford research group has demonstrated in three publications that protection from Ebolavirus can be achieved with existing pharmaceuticals.
Viruses consist of genetic material encapsulated in a protein coat. Elements of this protein coat are responsible for mediating entry of the virus into a host cell. The various ebolaviruses specifically use a glycoprotein trimer for essentially all functions of entry to a host cell, from attachment to membrane fusion. The critical importance of the glycoprotein and its subcomponents to ebolavirus infection make it of interest for controlling future epidemics: if the glycoprotein can be disrupted, Ebola loses its key to entering human cells.
The Oxford team started their research by crystallizing GP1, one of the components of the Ebola glycoprotein. By introducing pharmaceutical compounds and measuring the change in melting temperature of the protein, the binding strength of the compounds to the GP1 protein can be evaluated. Zhao et al conducted their first study in 2016, using the well-known painkiller ibuprofen and a selective estrogen receptor modulator used for breast cancer treatment called toremifene. They found that toremifene was particularly effective, reducing the melting temperature of the GP1 protein by 14°C at physiological pH and a concentration of 100 μM. The derived binding constant for toremifene based on this data becomes 16±4 μM, while ibuprofen was only hitting at 6±2 mM. The team was able to demonstrate that both agents were binding in a particular pocket on the GP1 protein.
In their 2017 study, Zhao et al chose a selection of eight compounds reported to have activity against Ebola, and repeated their thermal-shift assay with the new set of compounds. Four of the selected agents showed no affinity for the crystallized GP1, but the other four produced a significant effect. Their structures, and currently approved uses, are fairly diverse: bepridil is a calcium-channel blocker, sertraline and paroxetine are both selective serotonin reuptake inhibitors (SSRIs); and benztropine is a muscarinic antagonist prescribed to reduce extrapyramidal side effects. X-ray data showed that the same sub-pocket bound by ibuprofen and toremifene was the target for this set of drugs as well, with binding constants in the range of 0.29 – 1.3 mM. Recently, the same group has demonstrated that the antidepressants imipramine and clomipramine as well as the antipsychotic thioridazine are also capable of binding Ebola’s GP1 via the same sub-pocket.

The affinity of small molecules for the GP1 sub-pocket isn’t just a curiosity. In work funded by the Defense Threat Reduction Agency (DTRA), a team has tested some of these screening hits in mouse models to evaluate actual effectiveness. Over two studies, Lisa M. Johansen et al evaluated toremifene and the related drug clomipramine, as well as bepridil and sertraline. In mouse models, they found that dosing mice with toremifene led to a 50% survival rate against Ebolavirus, and clomipramine was particularly impressive, with a 90% survival rate. The antidepressant sertraline resulted in a 70% survival rate, but bepridil was the most impressive of all, with 100% of the mice surviving Ebola infection.
The work these two teams have done is an excellent lead on creating a true Ebolavirus treatment. While the high survival rates of the murine models in the DTRA studies is impressive, the drugs tested all had median inhibitory concentrations in the micromolar range, while typically drugs for use in humans only get to high nanomolar concentrations in vivo. The real utility of this research can come in conjunction with the structural analysis of the drug’s binding characteristics carried out by the Oxford team.
While an Ebola vaccine would be the preferred approach for preventing outbreaks, these two research teams have provided an unusually detailed look at what it would take to develop a structural inhibitor of Ebola glycoprotein by simply repurposing existing drugs that have a proven track record for decades.
Granted that murine studies do not always correlate with humans, but the creation of a small-molecule inhibitor, tailor-made to fit into the GP1 sub-pocket, may be a major step towards controlling the next Ebola outbreak when it occurs.
By Weston Mangin
Biomedical Engineer
HARDY DIAGNOSTICS